As the only National Cancer Institute-designated Comprehensive Cancer Center in Georgia, Winship is a leader in the treatment of head and neck cancer. Our staff conduct innovative research and clinical trials that are transforming how these cancers are identified, treated, and survived.
The radiation oncologists at Emory Proton Therapy Center work with the multidisciplinary Head and Neck cancer team at Winship, which includes experts in head and neck surgical oncology, reconstructive surgery, medical oncology, head and neck neuro-radiology, head and neck pathology, dentistry, supportive oncology, speech- language pathology, dieticians, social workers, physical therapy, and cancer rehabilitation. Your head and neck radiation oncologist will work closely with these other specialists to customize your head and neck cancer treatment plan and coordinate your care. We can also partner with a patient’s existing care team, whether they are across town or around the world.
Proton Therapy for Head and Neck Cancer
A head and neck cancer diagnosis can be one of the biggest challenges you and your family will ever face. Our team is dedicated to helping you meet that challenge through supportive care using the most advanced treatments available. Proton therapy may be a more precise radiation option for treatment of your cancer to help protect important functions like speech, swallowing, taste, hearing, vision, and voice. Our head and neck specialists will work with you to develop a personalized treatment plan which aims for fewer side effects and improved quality of life.
What We Treat
Head and neck cancers
- Oral cavity cancer (tongue, floor of mouth, buccal mucosa)
- Oropharyngeal cancers (base of tongue, tonsil, soft palate)
- Nasopharyngeal cancer
- Nasal cavity cancer
- Paranasal sinus cancer (maxillary, ethmoid, sphenoid, or frontal sinus)
- Salivary gland cancers (for example adenoid cystic carcinoma)
- Laryngeal cancer (vocal cords, epiglottis, “throat” cancer)
- Hypopharyngeal cancer (pyriform sinus)
- Head and neck sarcomas
- Re-irradiation
Benign (non-cancerous)
- Paraganglioma or Glomus Tumor
- Giant Cell Tumor
- Skull Base Meningiomas
Skull base cancers
- Chordoma
- Chondrosarcoma
- Esthesioneuroblastoma (olfactory neuroblastoma)
Comparison of Proton and X-Ray Therapy
Proton Therapy
Proton therapy is an extremely precise form of radiation treatment that can often better focus the radiation to match the shape and depth of the target. After treating the target, protons stop, avoiding exit dose radiation through the body. By reducing or avoiding radiation to sensitive normal healthy tissues and organs, proton therapy may reduce some of the side effects that can occur as a result of radiation treatments.
X-Ray Therapy
X-ray based radiation typically requires more beams or angles to deliver the radiation to the target. Unlike proton therapy where the radiation stops at the target, x-rays continue to deliver radiation as they exit through the body. As a result, x-ray based treatments typically result in increased radiation to normal healthy tissues and organs.
Proton Therapy Spares Radiation to the Mouth, Saliva Glands & Voice Box
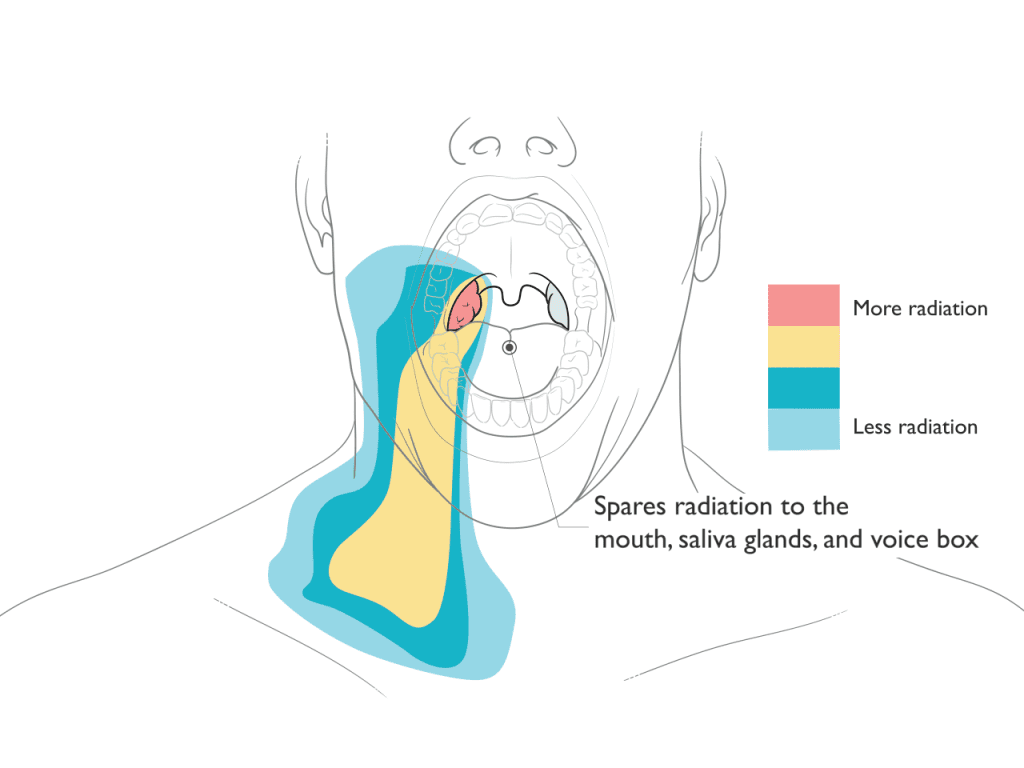
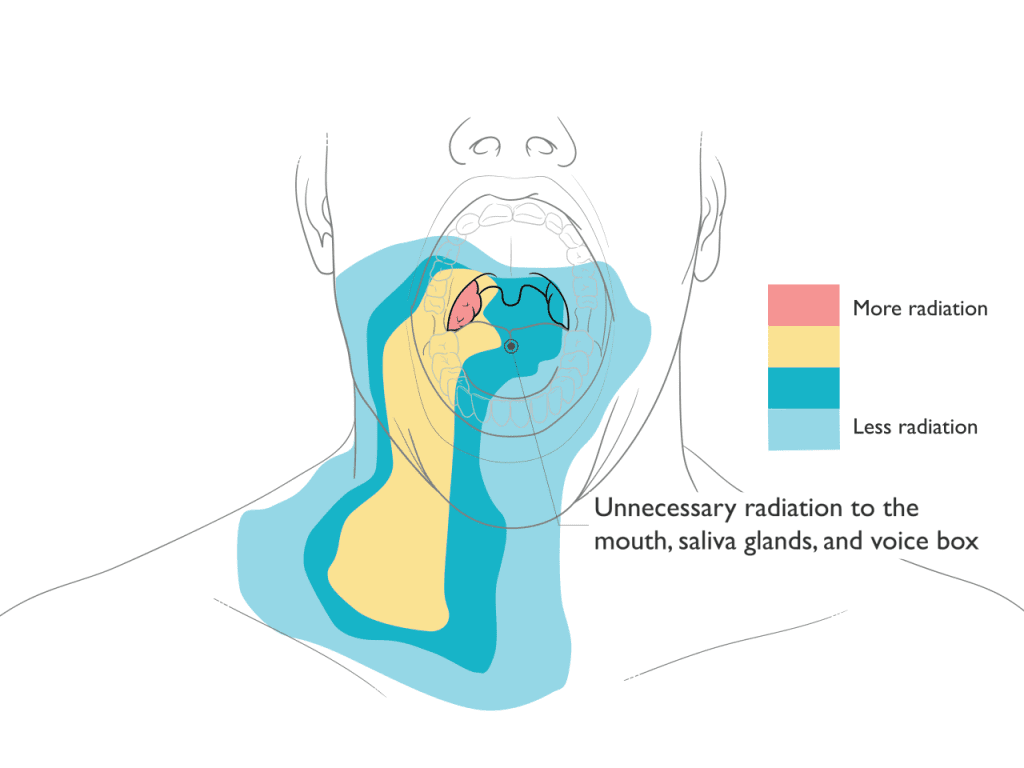
Benefits of Proton Therapy
In treatment of head and neck cancers, proton therapy can reduce or avoid radiation to surrounding healthy tissue and organs.
Depending on the tumor location and type, proton therapy may achieve the following benefits:
- Reduced risk of painful sores in the mouth (mucositis) during treatment.
- Reduced risk of dental decay after radiation.
- Reduced risk of problems swallowing (dysphagia or aspiration) during or after therapy.
- Reduced risk of hoarseness during treatment.
- Reduced risk of dry mouth (xerostomia) after radiation.
- Reduced risk of hearing loss after radiation. This is relevant for tumors near the cochlea, such as those in the nasopharynx, paranasal sinuses, or skull base.
- Reduced risk of hormone imbalances (endocrine dysfunction) which can particularly affect growth and development in children and young adults. This is relevant for tumors near the pituitary and hypothalamus, such as those in the nasopharynx, paranasal sinuses, or skull base.
- Reduced radiation to the bone marrow and circulating lymphocytes, which may help support the function of the immune system in fighting cancer.
- Reduced risk of developing a future second tumor or cancer, which is most relevant in younger patients, those with a good prognosis and a long life expectancy, and those patients who may have genetic conditions putting them at higher risk for developing other cancers.
Schedule a Consultation
What to Expect With Proton Therapy
The first step in your care is a consultation. During consultation, we review your medical history, perform a physical exam, decide if any additional tests are needed, discuss all radiation options that may be appropriate for your treatment plan, make recommendations, and answer questions.
To plan your treatment, you will undergo a “simulation” or planning session. During this visit our head and neck radiation therapists will help position you the way you will be treated each day. For patients receiving radiation treatment to the head and neck, a custom plastic mesh mask is made. This mask helps to get you in the correct position for treatment and fits snugly to remind you to hold still during treatment. You can see and breathe through the mask. A CT scan will be done to create a picture of you in the treatment position to design your radiation plan. Some patients also undergo an MRI during this visit to help identify the target for treatment. It normally takes 10 days for the team to design the proton treatment plan and perform the quality assurance checks before treatment begins.
Proton therapy is typically delivered once daily during weekdays, Monday through Friday. Most patients with head and neck cancers receive six to seven weeks of daily radiation. A few conditions can be treated in a shorter period of time. While some conditions are treated with radiation alone, proton therapy may be integrated with surgery, chemotherapy, immunotherapy, or other treatments as part of a comprehensive plan of care.
Like other types of radiation, proton therapy treatments are invisible and painless. Most head and neck radiation treatments average 30 minutes each day in the treatment room.
Patients are seen by the radiation oncology physician team weekly during treatment to monitor progress, answer questions, address concerns, and manage any side effects from treatment. Your radiation oncologist will discuss a plan to assess response to treatment and for long-term follow-up after therapy.
Studies on Proton Therapy in Head & Neck Cancer
Our team has identified these studies as examples of the clinical benefits of proton therapy in head and neck cancer.
Intensity Modulated Proton Therapy Versus Intensity Modulated Photon Radiation Therapy for Oropharyngeal Cancer: First Comparative Results of Patient-Reported Outcomes
This retrospective study of 81 patients treated with chemotherapy and radiation for oropharyngeal cancer compared patients reported outcomes between those treated with IMRT versus proton therapy. Patient- reported outcomes assess common symptoms of head and neck radiotherapy such as problems with taste, dry mouth, swallowing or chewing difficulties, lack of appetite, and fatigue. Both groups started with similar baseline symptoms. The average patient- reported symptom burden was statistically lower among those treated with proton therapy compared to IMRT during the first three months after treatment. These data suggest patients may report fewer and/or less intense symptoms during the recovery phase following treatment.
Comparative analysis of acute toxicities and patient- reported outcomes between intensity-modulated proton therapy (IMPT) and volumetric modulated arc therapy (VMAT) for the treatment of oropharyngeal cancer
This retrospective study of 305 patients receiving radiation for oropharyngeal cancer compared toxicities and patient reported outcomes between those treated with IMRT versus proton therapy. Those treated with proton therapy less often needed a feeding tube placed, were less often hospitalized after treatment, were less likely to need narcotic pain medications, and reported less cough, less altered taste, feeling less ill, and reported better swallow function.
Charged particle therapy versus photon therapy for paranasal sinus and nasal cavity malignant diseases: a systematic review and meta-analysis
This meta-analysis examined 41 studies and compared clinical outcomes of patients treated with particle therapy such as proton therapy with outcomes in those receiving photon therapy such as IMRT. At 5-years, both overall survival and disease-free survival were higher with particle therapy than with photon therapy. Focusing on those patients treated with IMRT versus proton therapy, proton therapy was associated with a significantly better disease-free survival at 5 years and local control at last follow-up. This may be related to an improved ability of proton therapy to adequately treat these complex tumors located near important critical structures such as the eyes, optic nerves, normal brain, and brainstem.
Acute toxicity in comprehensive head and neck radiation for nasopharynx and paranasal sinus cancers: cohort comparison of 3D conformal proton therapy and intensity- modulated radiation therapy
This retrospective study examined forty patients who received radiation treatment for tumors of the nasopharynx, nasal cavity, or paranasal sinuses including both sides of the neck, and compared toxicities of those treated with IMRT versus proton therapy. Those treated with proton therapy had, on average, a lower need for opioid pain medications at the completion of radiation and a lower rate of feeding tube dependence by the completion of radiation therapy and at 3 months after radiation. A higher radiation dose to the oral cavity and to the esophagus was correlated with an increased need for opioid pain medications. Proton therapy was associated with statistically significant lower average radiation doses to the oral cavity, esophagus, larynx (voicebox), and parotid salivary glands.
Comparative Effectiveness of Proton vs Photon Therapy as Part of Concurrent Chemoradiotherapy for Locally Advanced Cancer
This retrospective study examined nearly 1500 patients receiving chemotherapy and radiation for curable cancers of different disease sites, including head and neck cancers. A technique called propensity score weighting was used to account for differences in patient characteristics (patients treated with proton therapy tended to be older and to have a greater number of other serious health problems) and to minimize selection bias. Patients treated with proton therapy were significantly less likely to have a serious side effect in the first 90 days after treatment, and less often experienced a decline in their overall condition (performance status) during treatment. Patients treated with proton therapy were less likely to have an unplanned hospitalization.
Second cancer risk after primary cancer treatment with three-dimensional conformal, intensity-modulated, or proton beam radiation therapy
This study used the National Cancer Data Base (NCDB) to examine the frequency of developing a second cancer following radiation treatment for 9 different tumor types – including head and neck cancers – in 450,373 patients treated with X-rays or proton therapy. After adjusting for differences in patient age, follow-up duration, radiotherapy dose, use of chemotherapy, sociodemographic differences, and other factors, patients treated with proton therapy had a statistically significantly lower risk of developing a secondary cancer than those treated with X-ray therapy. This significant reduction in risk was seen despite the average follow-up time after radiation being only 5 years. The risk of secondary cancers increases with longer follow-up time after radiation, and it is encouraging to see this signal of reduced risk with proton therapy at an early timepoint.
Patient Stories
“I evaluated six treatment options before choosing Emory Proton Therapy Center. From the physicians to the front desk to the valet — the professionalism and care has been extraordinary at every single touchpoint. I’ve bragged about this place to everyone I know.”

“I’ve been through it, and I can’t say enough about the amazing care I received. The team who handled my treatments was absolutely wonderful, making a difficult time so much easier to navigate.”

My experience at Emory was incredible—it was as easy as drinking water! The therapy sessions only took about 5 to 10 minutes, and right after, I’d go for a 4-mile walk every single day. I had no side effects whatsoever—I can’t even tell that I had the treatment. Emory truly saved my life, and I couldn’t be more grateful.

Stephen, a 36-year old father from Columbus, Georgia, is one of the almost 2000 patients who have been treated at the Emory Proton Therapy Center since it opened in December 2018. He completed six weeks of proton therapy to treat a brain tumor.

“I went through 37 treatments for prostate cancer at the Emory Proton Center two years ago. The care I received from their team of professionals was amazing. I was willing to travel from South Carolina for treatment, and I’m so thankful I did. I started this fight in 2017 and today my PSA is still undetectable. Truly amazing folks.”

Proton therapy gave Zack his best shot at treating a spinal tumor that had come back. Zack was one of the first patients treated at the Emory Proton Therapy Center after it opened in 2018. The treatments, every weekday for six weeks, took less than one hour of his day and gave Zack the greatest odds of a long life with his wife and children.

Tony was diagnosed with prostate cancer in 2019 and sought care from experts at Emory Proton Therapy Center. He’s confident that the advanced radiation therapy gave him the best cancer treatment possible and says the comfort and care he got from Winship doctors and staff were unmatched. “There were many great solutions here in Atlanta, but the best to me was Emory Proton Therapy Center,” says Tony.




